Your Cart is Empty

YOUR CART
Your cart is empty!
Add your favorite items to your cart.
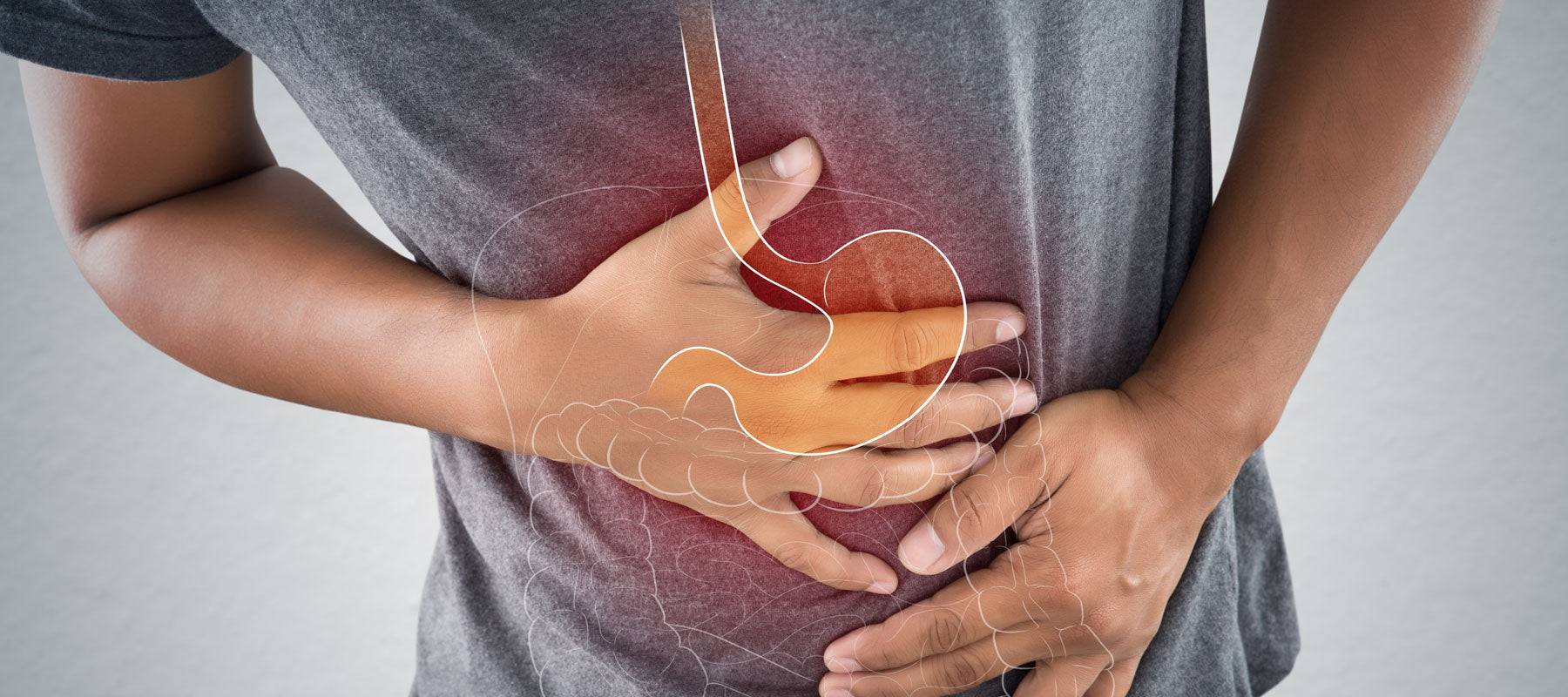
What is Acid Reflux and GERD?
March 28, 2018 7 min read
When you’re experiencing acid reflux, nothing is more important than relieving your symptoms. The heartburn, bitter taste, and other indications can affect your home life, work life, and basically your whole life. Our goal is to give you the tools to experience some relief and get your life back to normal.
In this post, we’ll answer high-level questions like, “what is acid reflux?” and “what causes acid reflux?”, discuss the nuanced differences between acid reflux vs. GERD, and finally, share some tips to help you find relief. Use the links below to navigate throughout the article, or read through for more detailed take on the topic.
Reflux 101: Understanding Acid Reflux and Finding Relief
Before we dive into acid reflux treatments, let’s establish some baseline knowledge — what is acid reflux, and why does it happen?
What is Acid Reflux?
We’ll start with a quick tour of the upper digestive tract to answer that question. Right above your stomach is a small valve called the LES, or lower esophageal sphincter. Normally, the LES only opens up to let food in and let air out (a.k.a burps). For most people, acid reflux occurs10 when the LES opens and lets stomach acid and semi-digested food flow back into the esophagus.

Heartburn11 (which, by the way, has nothing to do with the heart) is a symptom of both acid reflux and GERD and is caused by the acid eating away at the lining of the esophagus.
What Causes Acid Reflux?
As we mentioned, acid reflux (GER) and GERD occur when your lower esophageal sphincter does not function properly, allowing stomach contents, like stomach acid, to rise and permeate the esophagus. But how does the LES get to this state?
Diet, weight, stress, what you eat, when you eat, how much you eat, exercise, smoking, and genes, are just a few of the things that can promote acid reflux flare-ups. Body position, such as lying down or bending over, can also lead to an episode. Pregnancy can cause acid reflux as well, called gestational acid reflux. The growing baby creates less room for your stomach and the hormone progesterone causes muscles, like the LES, to relax. In some cases, a pregnancy pillow may provide some relief of nighttime acid reflux symptoms.

Acid Reflux vs. GERD
As an acid reflux sufferer, you may be familiar with the acronym GERD; in fact, acid reflux is also known as GER, gastro-esophageal reflux. GERD12 stands for gastro-esophageal reflux disease, which is the chronic form of acid reflux. If you experience acid reflux symptoms twice a week or more, you may actually have GERD.
Both acid reflux and GERD are commonly associated with heartburn, but there are a few key symptomatic differences to note when comparing acid reflux vs. GERD13.
- If you have acid reflux, you may taste stomach acid or partially digested food in the back of your mouth.
- Not all individuals with GERD have heartburn.
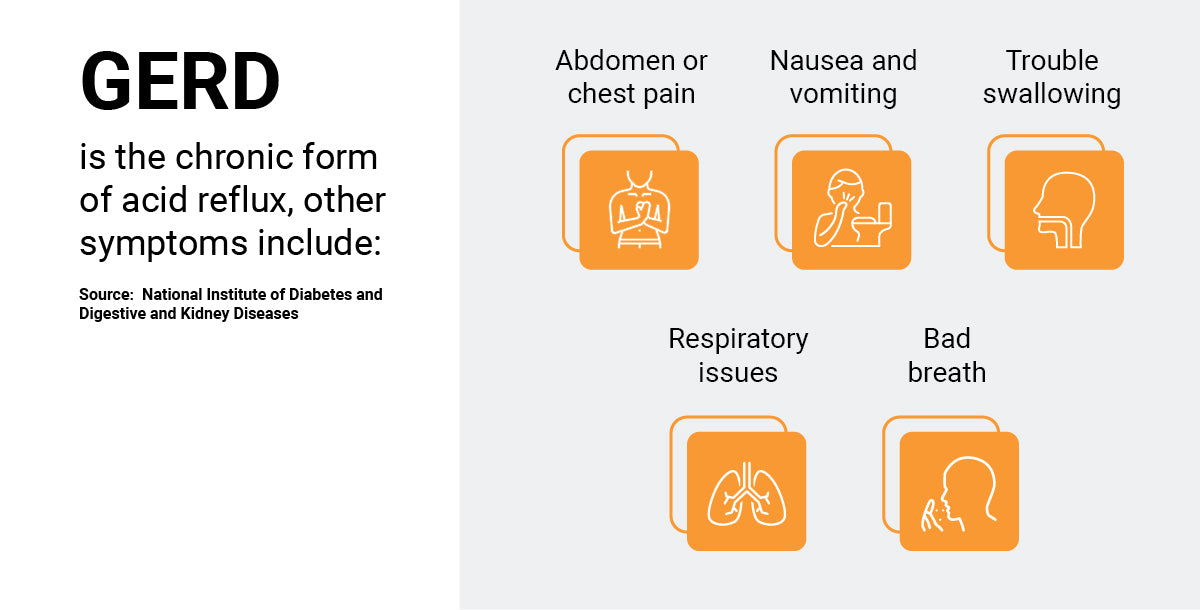
- Other symptoms of GERD include:
- Bad breath
- Nausea
- Abdomen or chest pain
- Trouble swallowing
- Respiratory issues
- Vomiting
Is it serious?
Everyone experiences acid reflux – an occasional episode is normal. However, GERD can be serious because of the acid that lingers in your esophagus. Over time, lingering acid causes inflammation and can create a precancerous condition known as Barrett’s Esophagus14. That’s not meant to scare you, but it’s important to know what acid reflux treatment measures you can take to be proactive.

Acid Reflux Treatments
The three mainstream ways to treat acid reflux/GERD are lifestyle changes, medication, and surgery. Lifestyle changes are always the first consideration. If that doesn’t work, your doctor may recommend over-the-counter or prescription medications. As a last resort, acid reflux surgery may be necessary.
Lifestyle Changes
There are many adjustments you can make that can help reduce acid reflux symptoms:
- Avoid trigger foods15: The known culprits are citrus fruits, onions, garlic, tomato-based products, spicy foods or sauces, fatty foods, fried foods, and chocolate, as well as peppermint-infused, caffeinated, or alcoholic beverages – some of these foods may not bother you while other foods not listed here may cause a reaction. It’s trial and error to find which foods trouble you the most.
- Incorporate GERD diet foods15: While certain ingredients can cause acid reflux flare-ups, other foods can actually help minimize your symptoms. High-fiber foods, alkaline-rich foods (melons, bananas, cauliflower), and watery foods (watermelon, lettuce, cucumber, broth) are known to prevent acid reflux. Additionally, milk, apple cider vinegar, and ginger can be used as home remedies for acid reflux.
- Lose weight: Recent studies16 have found that not only is GERD more common in individuals who are overweight or obese, but they’ve also proven weight loss to be an effective measure in resolving symptoms.
- Adjust mealtime habits: By simply changing how you eat, you may find acid reflux relief. The International Foundation for Gastrointestinal Disorders17 recommends opting for smaller meals to reduce symptoms, and avoiding eating within a couple hours of lying down. You can also try eating slowly, avoiding water and other fluids at mealtime, drinking plenty of water in between meals, taking short walks to help food settle, and chewing gum after a meal (avoid minty flavors).
- Sleep on an incline: Many individuals who struggle with GERD and acid reflux find that their symptoms intensify at night. This has to do with the role gravity plays within your body. When your body lies flat as you sleep, it’s working against gravity to push acid back into your stomach instead of allowing it to stay stagnant within your esophagus. Conversely, when you position yourself at an incline, gravity is working in your body’s favor, encouraging acid to relocate to your stomach where it belongs.
While everyone has their own tips for GERD and acid reflux treatment, the only two methods that are supported by objective clinical data are weight loss and sleeping at an incline. Taking into account that weight loss happens over a period of time, it’s a relief to know there’s a validated method that can be put to use immediately.
Multiple clinical studies support a drastic reduction in acid reflux exposure simply by sleeping inclined. Consider that acid clearance time (the time that it takes your body to naturally clear acid from the esophagus) can be improved by 67% when sleeping propped up at an angle. Some studies show a reduction in the total number of reflux episodes in this position. And an additional study states that 65% of people report less sleep disturbances.
Given that we developed an all-natural Acid Reflux Relief sleep system that goes beyond reducing acid reflux to helping you sleep soundly and comfortably, we hope you’ll consider MedCline as part of your overall strategy. Over the years, we’ve listened closely to feedback from physicians and reflux sufferers to develop the most effective, comfortable, and practical treatment possible.

Wrapping Up
- Acid reflux is when the LES opens and lets stomach acid and semi-digested food flow back into the esophagus.
- GERD is the chronic form of gastroesophageal reflux — symptoms may or may not include heartburn in addition to: bad breath, nausea, abdomen or chest pain, trouble swallowing, respiratory issues, and vomiting.
- The three main ways to treat acid reflux are:
- Lifestyle changes like losing weight, adjusting diet, and sleeping at an incline.
- Acid reflux medications — note: if medications are not effective for you, read up on GERD vs. NERD before talking to your doctor.
- Surgery
- Sleeping at an incline, specifically on the left side, is one of the most effective ways to reduce acid reflux symptoms. By propping your body up, residual acid can more easily be returned to your stomach.
- If you struggle with nighttime acid reflux, our Acid Reflux Relief System can help you get back to sleeping comfortably, reflux-free.
Say goodbye to nighttime Acid Reflux & GERD pain without sacrificing comfort.Related Product
Reflux Relief System
$249.99 BUY NOW
References:
Related Product
Reflux Relief System
$249.99
Say goodbye to nighttime Acid Reflux & GERD pain without sacrificing comfort.
Subscribe
Sign up to get the latest on sales, new releases and more …
Text SHOULDER to+1 (844) 942-0170to learn more and get discounts on our Shoulder Pain Relief System.
About MedCline
MedCline was founded in 2011 by Carl Melcher, M.D, who was a life-long sufferer of GERD. Dr. Melcher wanted to help the millions of GERD patients with a natural treatment alternative utilizing positional therapy. Since development, the Reflux Relief System has been validated in 7 clinical trials. Aiming to help other medical conditions with positional therapy, MedCline has also developed a Shoulder Relief System for those who suffer with chronic shoulder pain at night. Both MedCline Relief Systems are providing much-needed relief for those suffering from nocturnal acid reflux and/or nighttime shoulder pain to get quality, restorative sleep leading to a higher health-related quality of life.
To learn more about acid reflux relief, visit our Reflux Relief System Page.
To learn more about shoulder pain relief, visit our Shoulder Relief System Page.
